Cellulitis is a bacterial infection targeting deep skin layers and underlying tissue, with over 14 million cases annually in the U.S. Symptoms include skin redness, warmth, swelling, tenderness, and potential blisters.
Commonly affecting legs and feet, it arises from bacteria entering through skin breaks. Risk factors encompass age above 50, diabetes, and poor circulation. Diagnosis relies on clinical appearance, sometimes needing tests for specific bacteria identification.
Antibiotics are the primary treatment; severe cases may require hospitalization. Complications, though rare, can include bacteremia and osteomyelitis. Recovery is typically swift with antibiotics, but some cases need longer treatment or hospitalization.
Prevention focuses on avoiding injuries and managing conditions like diabetes. Immediate medical attention is crucial to avert complications.
Cellulitis appears as a red, swollen, and painful area of skin that is warm and tender to the touch. It is presumed to be due to staphylococci or streptococci infection and may be treated with cefazolin, cefuroxime, ceftriaxone, nafcillin, or oxacillin.Key Takeaways
1. Redness
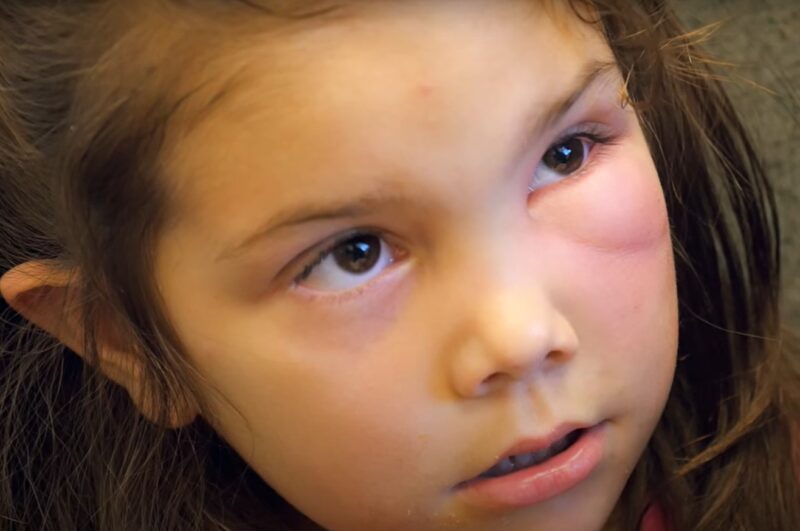
The redness is the result of increased blood flow to the affected area. Your body, recognizing the presence of bacteria, rushes white blood cells and other immune responses to the site, which results in inflammation.
The inflammation is your body’s attempt to isolate and eradicate the infection, but it also results in the skin becoming red, warm, and swollen.
Recognizing the redness early on is crucial. It’s the body’s way of sounding the alarm—a visual cue that prompts those affected to seek medical attention. Ignoring this sign can lead to the infection worsening, spreading, and potentially leading to severe complications.
Also, the first step is to consult a doctor so you can be sure about what condition to treat. Redness can be a sign of many issues. Besides cellulitis, it is one of the signs that could indicate the skin asthma.
It’s a mistake to underestimate the redness as a minor irritation; it’s the precursor to more serious symptoms and a clear indication that the body is under siege.
Steps to Treat Redness
- Antibiotic Treatment: If diagnosed with cellulitis, treatment usually involves antibiotics. The type and duration of antibiotic therapy can vary depending on the severity of the infection and the patient’s health history. It’s imperative to complete the entire course of antibiotics even if symptoms improve before the medication is finished to ensure the bacteria are fully eradicated.
- Care for the Affected Area: While undergoing treatment, keeping the infected area clean and protected helps prevent further irritation or infection. Gently washing with soap and water and covering with a sterile bandage can aid in recovery. Additionally, elevating the affected area can reduce swelling and redness.
- Monitor Symptoms: Throughout treatment, closely monitoring the redness and other symptoms is vital. If the area of redness continues to spread or if symptoms worsen, immediate communication with a healthcare provider is necessary. This could indicate that the infection is not responding to treatment and may require a different approach.
- Preventive Measures: After recovery, taking steps to prevent future occurrences is wise. This includes practicing good skin hygiene, promptly treating cuts or wounds, and keeping skin moisturized to avoid cracks or breaks where bacteria can enter.
2. Warmth
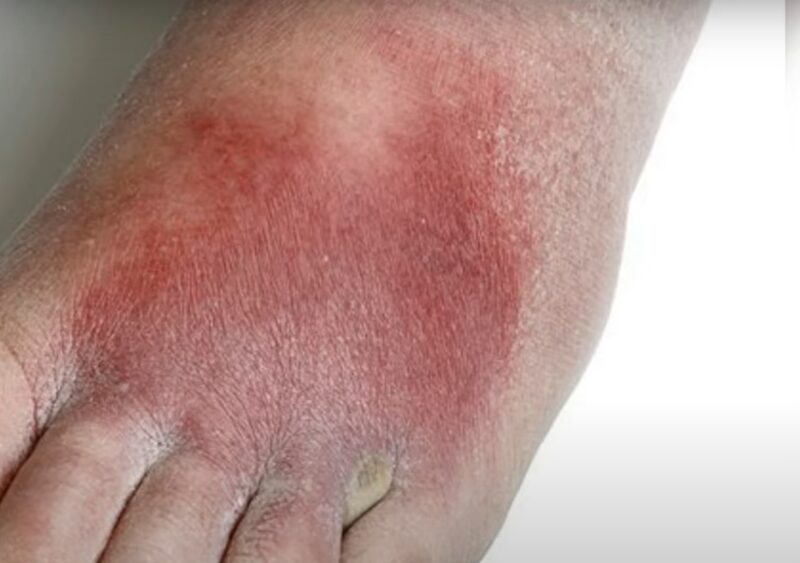
Warmth in the area affected by cellulitis is a direct consequence of the body’s inflammatory response to infection. When bacteria invade, the immune system kicks into high gear, increasing blood flow to the region.
This results in the affected area feeling notably warmer than surrounding tissues, a hallmark of the body’s attempt to isolate and neutralize the bacterial threat.
It helps to differentiate cellulitis from other skin conditions that might not present with the same level of localized heat. For those dealing with cellulitis, the warmth, combined with redness and swelling, can be uncomfortable and sometimes painful.
It’s a sign that should prompt immediate medical evaluation, as timely intervention can prevent the spread of infection and avoid complications.
Steps to Treat Warmth
- Follow Through with Prescribed Antibiotics: Effective treatment often includes antibiotics to fight the underlying bacterial infection. Completing the full course of antibiotics, even if symptoms improve, ensures the infection is thoroughly addressed.
- Apply Cool Compresses: While antibiotics work internally, applying cool compresses to the affected area can provide external relief from the warmth and discomfort. This should be done gently to avoid aggravating the skin.
- Elevate the Affected Limb: Elevation helps reduce blood flow to the inflamed area, potentially alleviating warmth along with swelling and redness.
- Rest and Hydration: Supporting the body’s immune system through adequate rest and hydration is beneficial in fighting the infection.
- Observe and Report Changes: Monitoring the warmth and other symptoms is important during treatment. Any increase in warmth or spreading of the heat could indicate that the infection is not responding to treatment, necessitating a review by a healthcare provider.
3. Swelling
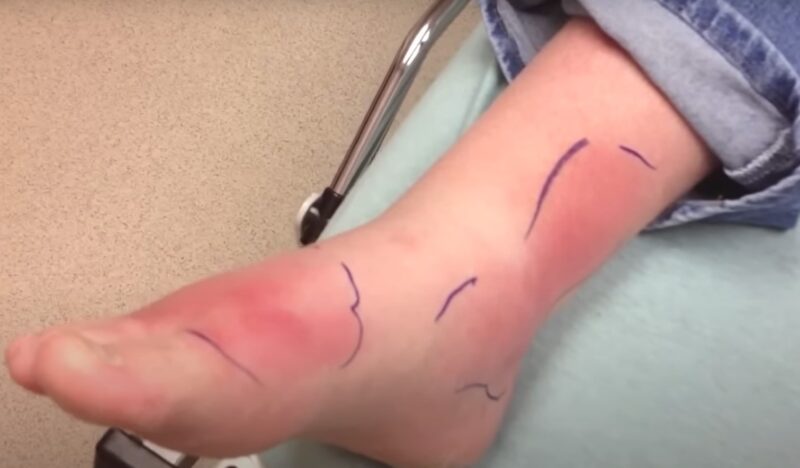
Swelling, or edema, in the context of cellulitis, is more than just an aesthetic concern; it’s a tangible manifestation of the body’s struggle against infection. This swelling occurs as the immune system responds to bacterial invaders, leading to an accumulation of fluid in the affected tissues.
The area not only looks swollen but may also feel tight and uncomfortable, significantly impacting mobility and daily activities, especially if the swelling is in the legs or arms.
The presence of swelling alongside redness and warmth underscores the severity of the infection. It’s a clear signal that the body is in distress, trying to contain the bacterial spread by increasing fluid in the tissue as part of the inflammatory process.
However, this natural defense mechanism also necessitates medical intervention to ensure that the infection is controlled and that the swelling does not lead to further complications.
Steps to Treat Swelling
- Antibiotics: They play a crucial role in reducing the bacterial load, which, in turn, can decrease swelling. It’s vital to take the full course of prescribed antibiotics to ensure effective treatment.
Valencia Higuera states that the treatment must be approached with caution, which means that monitoring of experts is essential. The types of medicine that can be prescribed are: Systemic antibiotics — oral antibiotics or, in severe cases, intravenous antibiotics — are needed to treat cellulitis.
- Elevate the Affected Area: Elevating the swollen area above heart level several times a day can help reduce swelling by promoting fluid drainage away from the affected tissues.
- Apply Cold Compresses: For immediate relief, cold compresses can be applied to the swollen area. This can help reduce inflammation and provide temporary relief from discomfort.
- Compression Garments: In some cases, healthcare providers may recommend wearing compression stockings or sleeves to help reduce swelling and support circulation.
- Limit Activity: Resting the affected area and avoiding strenuous activity can prevent further irritation and help reduce swelling.
- Monitor Progress: Keeping an eye on the swelling and other symptoms is essential during treatment. If swelling increases or spreads, it may indicate that the infection is not responding adequately to treatment, requiring further medical assessment.
- Manage Underlying Conditions: For individuals with conditions that predispose them to swelling, such as poor circulation or diabetes, managing these underlying issues is key to preventing recurrent cellulitis and associated swelling.
4. Tenderness
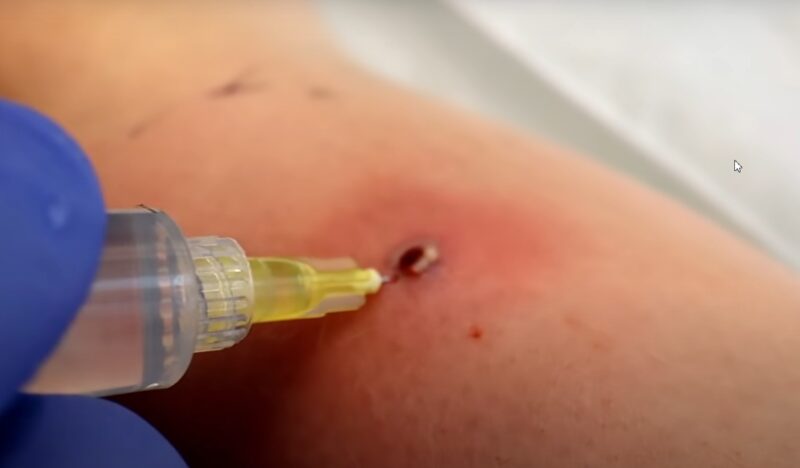
Tenderness in cellulitis is not just discomfort; it’s a piercing, often debilitating pain that arises from deep within the affected tissues. This symptom directly results from the body’s inflammatory response to the bacterial infection.
As the immune system fights off the invading bacteria, the area becomes not just swollen and warm, but also exquisitely sensitive to touch. The slightest pressure or contact can amplify the pain, making daily tasks and even restful sleep challenging.
It highlights the severity of cellulitis and the urgency of seeking medical intervention. Not only does it affect physical well-being, but it also impacts emotional and psychological health, as the persistent pain can be distressing and exhausting.
Steps to Treat Tenderness
- Complete Antibiotic Course: Prescribed antibiotics target the root cause of tenderness—the bacterial infection. It’s crucial to adhere to the prescribed regimen, completing the full course to ensure the infection is fully addressed.
- Pain Management: Over-the-counter pain relievers, such as acetaminophen or ibuprofen, can be used to alleviate tenderness and discomfort. Always consult with a healthcare provider before starting any medication to ensure it’s safe and appropriate for your situation.
- Rest and Protect the Area: Minimizing movement and avoiding pressure on the affected area can help reduce tenderness. Resting and protecting the area from contact or injury is important for healing.
- Apply Warm Compresses: Contrary to cold compresses for swelling, warm compresses can soothe the tender area, promoting circulation and providing relief from pain.
- Monitor Symptoms: Keeping track of the tenderness and associated symptoms is important during treatment. If pain escalates or fails to improve with treatment, this may require reevaluation by a healthcare professional.
- Follow Up: Even after symptoms improve, follow-up appointments with a healthcare provider are important to ensure the infection has been fully resolved and to address any lingering tenderness or pain.
5. Blisters
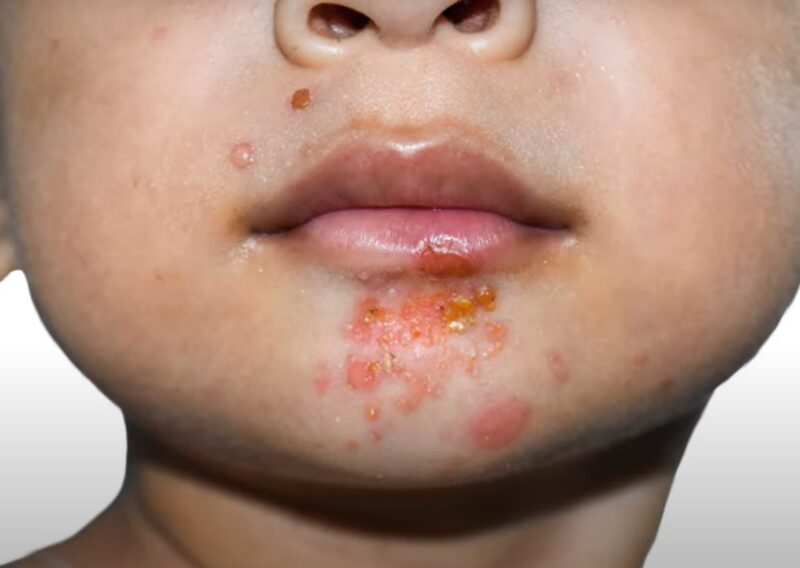
These fluid-filled sacs form as a defense mechanism, with the body attempting to cushion and protect the underlying tissue from further bacterial assault. However, blisters also signify that the infection has created significant tissue damage and inflammation.
They can vary in size and may appear as clear, fluid-filled, or pus-filled, indicating a more advanced infection stage.
The development of blisters in cellulitis is a significant concern. It not only suggests a deeper or more aggressive infection but also increases the risk of complications. Blisters can rupture, providing an entry point for additional bacteria and complicating the healing process.
Steps to Treat Blisters
- Antibiotic Therapy: Enhanced antibiotic treatment may be necessary when blisters are present. This could mean a stronger or longer course of antibiotics, and in some cases, intravenous antibiotics if the infection is particularly severe.
- Do Not Pop or Drain Blisters: It’s crucial to leave blisters intact to reduce the risk of further infection. Popping or draining them without medical supervision can lead to complications.
- Protective Covering: If advised by a healthcare provider, applying a sterile bandage can protect blisters from accidental rupture and keep the area clean.
- Elevate and Rest the Affected Area: Reducing pressure on and movement of the affected area can prevent blisters from rupturing prematurely and help reduce swelling and discomfort.
- Pain Management: Pain associated with blisters can be significant. Over-the-counter pain relief, as recommended by a healthcare provider, can help manage discomfort.
- Follow Up and Monitor for Infection: Regular follow-up with a healthcare provider is essential to ensure the infection is responding to treatment. Monitoring the blisters for signs of increased redness, pus, or additional swelling is crucial.
- Hygiene and Care: Keeping the area clean and dry is important. Changes in bandages should be done as advised by a healthcare professional, ensuring hands and materials are sterile to avoid introducing new bacteria.
6. Peau d’Orange Appearance
The term “peau d’orange,” French for “orange peel,” describes a distinct texture of the skin that resembles the surface of an orange. This symptom of cellulitis is characterized by dimpling or pitting of the skin.
It occurs when edema, or swelling beneath the skin, pushes against the connective tissue, creating a bumpy surface.
The peau d’orange appearance is a clear indication that the infection has affected the lymphatic system, leading to fluid buildup and inflammation.
The involvement of the lymphatic system can complicate the treatment of cellulitis, as it indicates that the body’s fluid drainage system is compromised.
Steps to Treat Peau d’Orange Appearance
- Antibiotic Treatment: Given the advanced nature of cellulitis indicated by peau d’orange, a robust antibiotic regimen is often necessary. This might include oral or, in more severe cases, intravenous antibiotics to combat the infection effectively.
- Manual Lymph Drainage: In some cases, healthcare providers may recommend manual lymph drainage therapy. This specialized form of massage can help stimulate the lymphatic system, encouraging the drainage of built-up fluid and reducing swelling.
- Compression Therapy: Wearing compression garments can support the affected area, helping to reduce swelling and improve lymphatic drainage. These garments should be used under the guidance of a healthcare professional.
- Elevate the Affected Limb: Keeping the affected area elevated can help reduce fluid buildup and alleviate the peau d’orange appearance. This is particularly effective for limbs.
- Monitor for Changes: Regular monitoring of the skin’s appearance and texture is important. Any worsening of the condition should be reported to a healthcare provider immediately.
- Skin Care: Maintaining the cleanliness and integrity of the skin is vital. Gentle washing and moisturizing can help protect the skin and support healing.
FAQs
Can cellulitis heal without treatment?
Cellulitis is a serious bacterial infection that can spread quickly to the lymph nodes and bloodstream if untreated. It is very important to seek medical attention and take antibiotics as soon as possible.
How can I prevent cellulitis early?
You can prevent cellulitis by keeping your skin clean and healthy, avoiding injuries and infections, and treating any chronic skin conditions. If you have a wound, wash it with soap and water, cover it with a bandage, and change it regularly.
What foods prevent cellulitis?
There is no specific diet that can prevent cellulitis, but eating a balanced and nutritious diet can help boost your immune system and fight infections. Some foods that may be beneficial are green leafy vegetables, fresh fruits, nuts, seeds, garlic, ginger, and cranberries.
Does drinking a lot of water help with cellulitis?
Drinking a lot of water can help flush away the toxins and bacteria from your body and keep your skin hydrated. It can also reduce inflammation and swelling caused by cellulitis. You should drink at least eight glasses of water per day.
Last Words
Early detection of cellulitis symptoms is key to preventing further health complications. Recognizing changes in skin appearance, warmth, and texture can lead to prompt medical evaluation. Proactive attention to these signs supports effective management of the condition.

